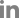Non-regenerative anemia with a suspected immune-mediated pathogenesis has been reported in more than 250 dogs [
1-
4]. It was classified as precursor-targeted immune-mediated anemia (PIMA) in 2 studies [
5,
6]. PIMA is a hematologic disease characterized by ineffective erythropoiesis. PIMA primarily involves an immune-mediated attack on the erythroid precursor in the bone marrow, which is distinctly different from immune-mediated hemolytic anemia (IMHA) with destruction of peripheral or mature red blood cell (RBC) [
5-
7]. Bone marrow should be evaluated to make a definitive diagnosis as PIMA and immunosuppressant drugs are needed as therapeutic measures for longer period than in IMHA [
5,
6]. In this case report, we performed a bone marrow examination for a definitive diagnosis of PIMA, administered a combination of 2 immunosuppressants (prednisolone [PDS] and mycophenolate mofetil [MMF]), and achieved complete remission.
A 13-year-old (weight, 3.8 kg) neutered male Maltese dog presented to our referral hospital with a 3-week history of depression and anorexia. Physical examination revealed a body condition score of 4/9, rectal temperature of 38.5°C, heart rate of 150 beats per minute, respiratory rate of 24 per minute, systolic blood pressure of 120 mmHg (doppler method), and pale mucus membrane. Laboratory investigations, including complete blood count (CBC) and serum chemistry, were performed using blood samples from jugular vein. CBC revealed non-regenerative anemia (hematocrit [HCT], 12.9%; reference interval, 37.3%-61.7%; reticulocyte count [Retic], 12.8 K/μL; reference interval, 10.0-110.0 K/μL). Other values of CBC (white blood cell and platelet counts), and serum chemistry profiles were within their reference intervals. By peripheral blood smear, marked spherocytosis (more than 5 spherocytes per high-power field) were observed (
Fig. 1). In addition, the polymerase chain reaction test results for canine anemia panel including anaplasma, ehrlichia, babesia, leptospira, bartonella, hemotropic mycoplasma, and rickettsia spp. (POBGEN Canine Anemia Pathogen Test; Pobanilab, Korea) were all negative. And, thoracic radiography and abdominal ultrasonography revealed nonspecific findings. Therefore, we tentatively diagnosed the dog as late-stage IMHA with iron deficiency or PIMA. The dog received a transfusion with packed RBC (10 mL/kg for 4 hours) to relieve tissue hypoxia and ischemia and was administered PDS (Solondo; Yuhan Pharm, Korea) at 1 mg/kg per oral (PO) q 12 hours, and MMF (Cellcept; Roche Pharm, Korea) at a dose of 10 mg/kg PO q 12 hours on the first day of admission. In addition, clopidogrel (Pidogul; Hanmi Pharm, Korea) at 2 mg/kg PO q 24 hours to prevent thromboembolism.
On day 4, CBC showed that remained non-regenerative anemia (HCT, 21.7%; Retic 15.4 K/μL), and bone marrow core biopsy was performed to make a definitive diagnosis. The marrow cellularity was moderate (greater than 60% cells and less than 40% fat) with a moderate amount of iron pigment. The myeloid:erythroid ratio was approximately 1:1, low in favor of erythroid cells, indicating erythroid hypercellularity. The maturation of the myeloid series was complete, orderly and morphologically unremarkable. In addition, mild collagen myelofibrosis was present. The overall findings were consistent with late-stage PIMA (
Fig. 2). Therefore, immunosuppressants (PDS and MMF) were remained for the dog.
The Retic exceeded the normal interval on day 27 (207 K/μL) with increased HCT (26.4%). Furthermore, the dog achieved complete remission from anemia on day 88 (HCT, 37.6%; Retic, 96.3 K/μL). We continued to prescribe the 2 immunosuppressants (PDS and MMF) for 517 days, and tapered the dosage according to the hematologic value. Approximately 120 days after withdrawal PDS and MMF, Day 622 was the last follow-up of the dog, and PCV was normal (41.5%).
The diagnostic criteria for PIMA have been proposed as follow: (1) Persistent non-regenerative anemia (HCT ≤ 30%; Retic < 6 K/μL) should last for at least 5 days. (2) Bone marrow cytologic or histologic findings should reveal ineffective bone marrow erythropoiesis, and decreased myeloid:erythroid ratio with erythroid hypercellularity. (3) Other cell lines including white blood cells and platelets should have no dysplastic features in bone marrow biopsy [
5-
7]. This case was consistent with this criteria.
Assenmacher et al. [
5] have reported that only 2% of PIMA dogs (2 of 66 cases) showed spherocytosis in peripheral blood smear. Interestingly, the dog in this report showed marked spherocytosis, and it might be evidence of hemolysis related to various antibodies or shared epitopes in developing erythroid and mature red blood cells.
The dog was managed with PDS and MMF for 517 days. In previous studies, PIMA dogs were administered immunosuppressive drugs including prednisone, cyclosporine, and azathioprine [
5,
6]. The median resolution time was 178 days, and the median survival time was 578 days for myelofibrosis [
5]. In this case, the resolution time was 88 days, and the total duration of follow-up was 622 days. Combination of PDS and MMF might be an additional effective therapeutic option.
A previous study have reported that regenerative response in PIMA dogs might be delayed when collagen myelofibrosis (chronic inflammatory state) was detected by bone marrow examination [
5]. Another study also have reported that the median survival time of PIMA dogs without collagen myelofibrosis (1,429 days) was significantly longer than that of PIMA dogs with collagen myelofibrosis (578 days) [
6]. The dog in this report also had mild collagen myelofibrosis, and took 27 days to achieve bone marrow remission.
Herein, we have shown here a late-stage PIMA dog definitively diagnosed by bone marrow core biopsy. Also, the dog was administered a combination of 2 immunosuppressants (PDS and MMF), and achieved complete remission.
Acknowledgments
This study was funded by the National Research Foundation (NRF) of Korea grant funded by the Korea government (MSIT) (2021R1F1A1063399).
Fig. 1.
Peripheral blood smear with hematoxylin and eosin staining. It revealed marked spherocytosis (more than 5 spherocytes per high-power field). Scale bars: (A) 20 μm and (B) 100 μm.
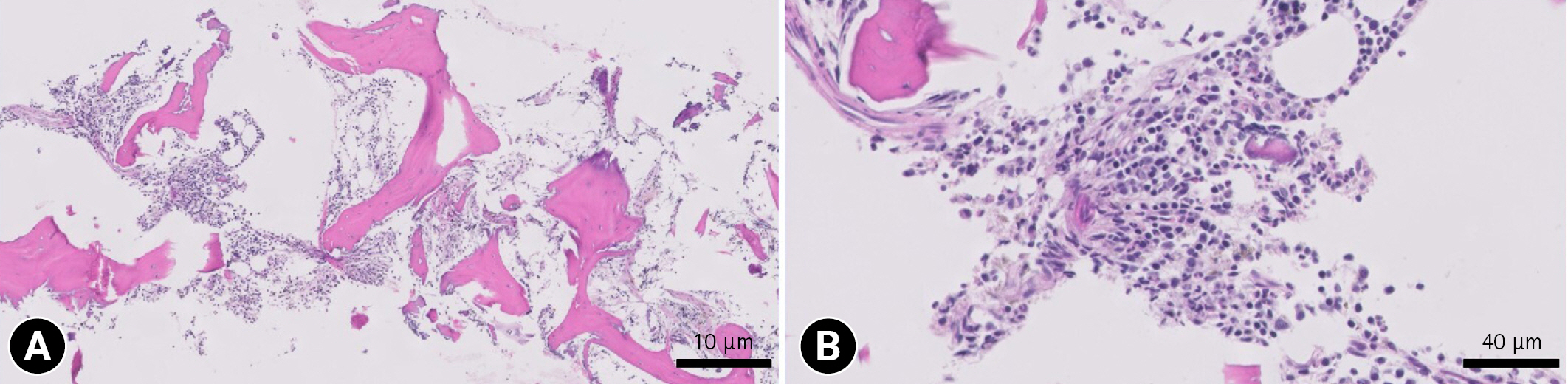
Fig. 2.
Bone marrow examination with hematoxylin and eosin staining. The marrow cellularity was moderate with a moderate amount of iron pigment. It also revealed erythroid hypercellularity with mild myelofibrosis. Scale bars: (A) 10 μm and (B) 40 μm.
References
1. Weiss DJ. Bone marrow pathology in dogs and cats with non-regenerative immune-mediated haemolytic anaemia and pure red cell aplasia. J Comp Pathol 2008;138:46-53.


2. McManus PM, Craig LE. Correlation between leukocytosis and necropsy findings in dogs with immune-mediated hemolytic anemia: 34 cases (1994-1999). J Am Vet Med Assoc 2001;218:1308-1313.


3. Weinkle TK, Center SA, Randolph JF, Warner KL, Barr SC, Erb HN. Evaluation of prognostic factors, survival rates, and treatment protocols for immune-mediated hemolytic anemia in dogs: 151 cases (1993-2002). J Am Vet Med Assoc 2005;226:1869-1880.


5. Assenmacher TD, Jutkowitz LA, Koenigshof AM, de A Lucidi C, Scott MA. Clinical features of precursor-targeted immune-mediated anemia in dogs: 66 cases (2004-2013). J Am Vet Med Assoc 2019;255:366-376.















 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print